Sarcoptic mange in pets is a highly contagious skin condition that affects both dogs and cats. Also known as scabies, this parasitic infection is caused by microscopic mites that burrow into the outer layers of your pet’s skin. Once there, the mites live, reproduce, and lay eggs, triggering a strong allergic reaction that leads to intense itching, discomfort, and visible skin changes. While sarcoptic mange in pets can look alarming and may spread quickly, the good news is that this condition is treatable and curable when recognized early and managed with appropriate veterinary care.

Key Takeaways
- Sarcoptic mange (scabies) is a highly contagious parasitic skin disease caused by burrowing mites.
- In dogs, it is caused by Sarcoptes scabiei; in cats, a closely related mite (Notoedres cati) causes a similar condition.
- The disease spreads mainly through direct contact with infected animals.
- Sarcoptic mange is zoonotic, meaning people may develop a temporary itchy rash, which usually resolves once the pet is treated.
What is Sarcoptic Mange?
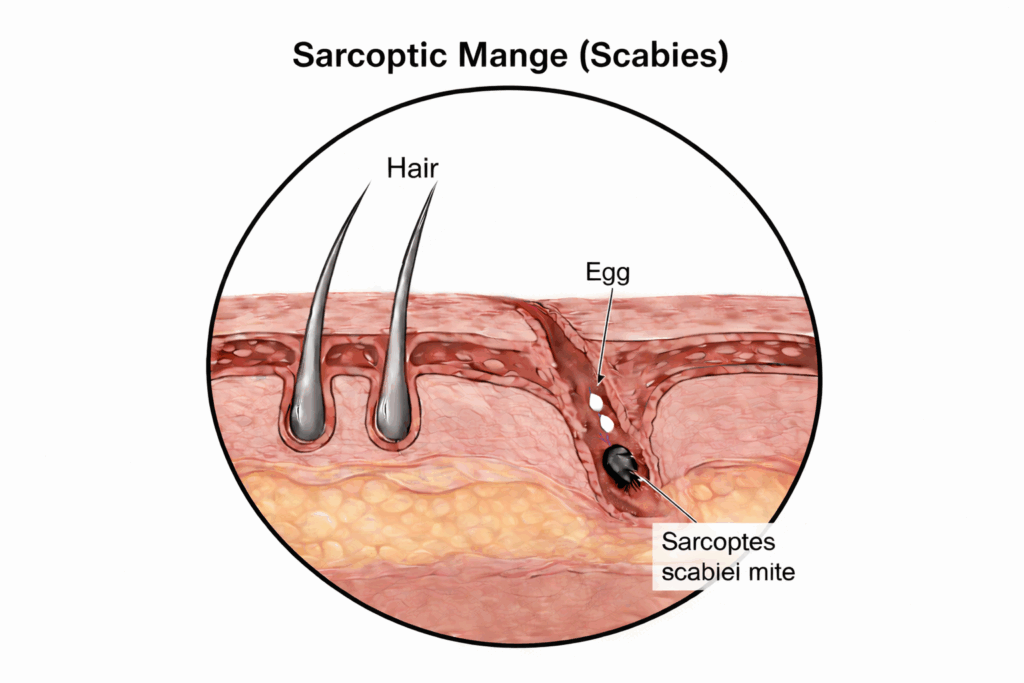
Sarcoptic mange, also known as scabies, is a highly contagious skin condition caused by parasitic mites that burrow into the outer layers of a pet’s skin (1, 2). Once there, the mites live, reproduce, and lay eggs. Their presence triggers a strong allergic reaction, leading to intense itching, discomfort, and visible skin changes (3).
- In dogs, sarcoptic mange is caused by Sarcoptes scabiei (4)
- In cats, a closely related mite called Notoedres cati causes a similar condition, often referred to as feline scabies (4)
While the condition can look alarming and may spread quickly, the good news is that sarcoptic mange is treatable and curable when recognised early and managed appropriately with veterinary care.
How do Pets Catch Sarcoptic Mange?

Sarcoptic mange spreads mainly through direct contact with infected animals. Less commonly, short-term contact with contaminated items such as bedding, collars, or grooming tools may also contribute to spread (1, 5).
Common situations where pets may be exposed include:
- Contact with infected animals at parks, day care, boarding kennels, grooming facilities or shelters (5, 6)
- Living in multi-pet households (6)
- Contact with wildlife, such as foxes (particularly for dogs) (5)
One of the challenges with sarcoptic mange is that pets can be contagious before showing obvious signs. This allows mites to spread unnoticed if only visibly itchy animals are treated (11).
It’s important to note that sarcoptic mange is not caused by poor hygiene and can affect pets that are otherwise healthy and well cared for. However, animals with weakened immune systems, underlying medical conditions, or advanced age may be more susceptible or develop more severe symptoms (7). Males and females are affected equally, and there is no breed predisposition (1).
Why Sarcoptic Mange Matters for Pet Owners

Sarcoptic mange is zoonotic, meaning it can affect people who have close contact with an infected pet. In humans, exposure may cause an itchy, red, bumpy rash, with itchiness sometimes worse at night. Affected areas commonly include the arms, wrists, waist, abdomen or where the skin has had close contact with the pet (8, 9). Importantly, the animal mite cannot reproduce on human skin. Therefore, symptoms are usually self-limiting and resolve once the pet has been treated and environmental exposure is reduced, however consult your doctor for advice (7, 9).
Signs of Sarcoptic Mange to Watch for

The most noticeable sign of sarcoptic mange is intense itching, which often begins weeks after exposure and tends to worsen over time.
Top 5 signs to look out for include:
- Persistent scratching, chewing, or rubbing (1)
- Red, inflamed skin (1, 2)
- Scaly crusts, scabs, or thickened skin (1, 2)
- Hair loss (1, 2)
- Skin sores or secondary infections caused by scratching (1)
Lesions tend to follow a characteristic pattern, usually starting on areas with less hair (10). These include:
- The edges of the ears
- Elbows and hocks
- Abdomen and chest
- The face and around the eyes
As the condition progresses, larger areas of the body may become affected (10). Without treatment, itching can become severe and widespread, significantly impacting a pet’s comfort and quality of life.
How do Veterinarians Diagnose Sarcoptic Mange?
Diagnosing sarcoptic mange can be challenging, as the mites are difficult to find and no single test that detects every case.

Veterinarians often rely on a combination of:
- Superficial skin scrapings and cytology to demonstrate the presence of mites, their eggs or waste material under a microscope (1, 6)
- Assessment of clinical signs and the distribution of skin lesions (1)
- A treatment trial may be used, where medication is started based on strong suspicion and the pet’s response is monitored. This approach is often used because mites are difficult to detect early and sarcoptic mange can resemble food or environmental allergies, contact reactions to grass, and other parasitic conditions such as ear mites (1, 6, 11)
What Does Treatment of Scabies Typically Involve?

Sarcoptic mange is highly treatable with modern veterinary medications. Treatment focuses on:
- Eliminating the mites
- Reducing itching and inflammation
- Treating any secondary skin infections, if present
- Preventing reinfestation
Medical treatment commonly includes:
- Prescription spot-on or oral antiparasitic medications (5, 7)
- Anti-itch treatments to improve comfort during recovery (6)
- Antibiotics or antifungal medications if secondary infections are identified (6)
A key part of successful treatment is a “treat-all” approach. All pets in the household should be treated at the same time, even if they are not showing symptoms. Treating only the visibly affected pet often leads to reinfestation (6). Consult your veterinarian on the best treatment and approach for your pet.
Some pets may appear itchier during the first week of treatment as the mites die, but this reaction is usually temporary. Most pets show noticeable improvement within 2 weeks, although full skin healing and hair regrowth may take longer (6).
Can Scabies be Prevented?

While exposure to sarcoptic mange cannot always be avoided, pet owners can help reduce the risk by:
- Using routine parasite prevention as recommended by their veterinarian
- Avoiding close contact with animals showing signs of skin disease
- Seeking veterinary advice promptly if a pet develops sudden or intense itching (12)
- Keeping bedding, collars, and grooming tools clean (12)
At room temperature and moderate humidity, sarcoptic mites usually survive only 24–36 hours away from a host. As a result, extensive cleaning of the home is not usually necessary. In cooler or more humid environments, mites may persist slightly longer. Simple measures, such as washing pet bedding, blankets, and frequently used items, are usually sufficient to reduce the risk of reinfestation, especially in multi-pet households (13).
What Options Can Pet Owners Explore if Their Cat or Dog Has Sarcoptic Mange?

A diagnosis of sarcoptic mange can feel overwhelming, but effective treatment and support are available.
Pet owners can:
- Work closely with their veterinarian to create a treatment and follow-up plan
- Discuss ongoing parasite prevention strategies to reduce future risk
- Ask about short-term medications to help manage itching and discomfort during recovery
- Consider pet insurance coverage to help manage unexpected veterinary costs
Early diagnosis and prompt treatment not only improve your pet’s comfort but also help limit the spread to other animals and people.
References
- Dumitrache MO, Cadiergues MC. The most effective systemic treatment in dogs with sarcoptic mange: a critically appraised topic. BMC Vet Res. 2023 Oct 5;19(1):189.
- Niedringhaus KD, Brown JD, Sweeley KM, Yabsley MJ. A review of sarcoptic mange in North American wildlife. International Journal for Parasitology: Parasites and Wildlife. 2019 Aug;9:285–97.
- Colombo M, Morelli S, Sacra M, Trezza G, Paoletti B, Traversa D, et al. An Uncommon and Severe Clinical Case of Sarcoptes scabiei Infestation in a Cat. Pathogens. 2022 Dec 30;12(1):62.
- Malik R, Stewart KM, Sousa CA, Krockenberger MB, Pope S, Ihrke P, et al. Crusted scabies (sarcoptic mange) in four cats due to Sarcoptes scabiei infestation. Journal of Feline Medicine and Surgery. 2006 Oct;8(5):327–39.
- Krieger K, Heine J, Dumont P, Hellmann K. Efficacy and safety of imidacloprid 10% plus moxidectin 2.5% spot-on in the treatment of sarcoptic mange and otoacariosis in dogs: results af a European field study. Parasitol Res. 2005 Oct;97(S1):S81–8.
- Cornell University College of Veterinary Medicine. Sarcoptic mange (scabies) [Internet]. Ithaca (NY): Cornell University; [cited 2026 Jan 16]. Available from: https://www.vet.cornell.edu/departments-centers-and-institutes/riney-canine-health-center/canine-health-topics/sarcoptic-mange-scabies
- Hampel V, Knaus M, Schäfer J, Beugnet F, Rehbein S. Treatment of canine sarcoptic mange with afoxolaner (NexGard® ) and afoxolaner plus milbemycin oxime (NexGard Spectra® ) chewable tablets: efficacy under field conditions in Portugal and Germany. Parasite. 2018;25:63.
- Mitchell E, Wallace M, Marshall J, Whitfeld M, Romani L. Scabies: current knowledge and future directions. Front Trop Dis. 2024 July 23;5:1429266.
- Department of Health, Victoria. Scabies control guidelines [Internet]. Melbourne: Health Victoria; Reviewed 10 Jul 2024 [cited 2025 Jan 16]. Available from: https://www.health.vic.gov.au/infectious-diseases/scabies-control-guidelines.
- Thomson P, O N, Ez A. Main mites associated with dermatopathies present in dogs and other members of the Canidae family. Open Vet J. 2023;13(2):131.
- Miller WH, Griffin GE, Campbell KL, Muller G, Kirk RW. Muller & Kirk’s small animal dermatology. 7th edition. St. Louis, Mo: Elsevier/Saunders; 2013. 938 p.
- Veterinary Partner. An overview of sarcoptic mange (scabies) in dogs [Internet]. Veterinary Information Network (VIN); 2023 Aug 24 [cited 2026 Jan 16]. Available from: https://veterinarypartner.vin.com/doc/?id=4951492&pid=19239
- Ong CY, Vasanwala FF. Infected with Scabies Again? Focus in Management in Long-Term Care Facilities. Diseases. 2018 Dec 29;7(1):3.


